“We are able to uncover complex control circuits that lead from salt intake to immune deficiency”
…with these words Prof. Christian Kurts from the University of Bonn on March 25, 2020 joined a long list of scientists who have raised the alarm yet again to the dangers of dietary salt. This warning is especially timely in the context of the present pandemic of COVID-19. As we all want to reduce the chances of contracting or dying from COVID-19, one area that deserves more focus is the understanding of the interplay between dietary salt and the immune system.
Presence of comorbidities, especially hypertension, a very important salt linked health problem, has been the hallmark of the mortalities from COVID-19. This also explains why Black Americans, who are among the most salt sensitive groups, have had a disproportionately high mortality from COVID-19.
One of the landmark publications from which we drew the attention in our writing in 2013 “Salt: Friendly Fire Aimed at You” was based on research jointly published from the prestigious universities of Yale, MIT and Harvard. In this publication the interplay between table salt and the immune system resulted in incremental production of auto immune protein in response to salt. Special thymic lymphocytes labeled Th17 cells proliferated and produced more autoimmune proteins in vitro and in experimental animals. Mice genetically engineered to get multiple sclerosis manifested the disease quicker and more aggressively in response to salt. This pathway is likely responsible of more rigorous auto immune response to COVID-19 which affects multi-organ systems once infected. This phenomenon would explain higher mortality from COVID-19 among hypertensives, especially salt sensitive Black Americans.
Writing on the relationships between salt and dementia, we also reported in 2015 the finding of these autoimmune proteins causing neuronal degeneration which is a key feature of Alzheimer’s dementia. In a subsequent writing, we reported on a landmark study linking dietary salt to excess production of glucocorticoids. This study published from Vanderbilt University shows the pathway from table salt to metabolic syndrome, including development of type 2 diabetes.
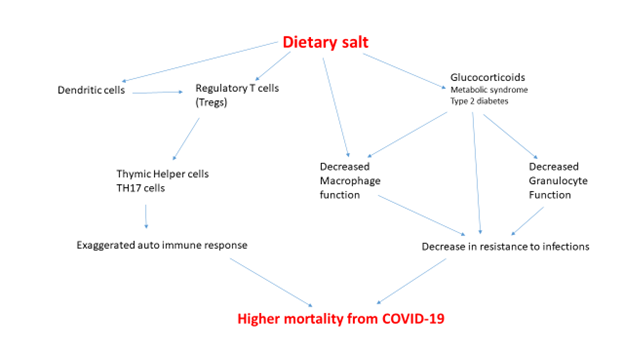
Several published reports also established the relationship of excess production of glucocorticoids in response to dietary salt. The interaction between the immune system and salt is in part mediated via excess glucocorticoids which are known to decrease the immune response. The current research from University of Bonn and other institutions is summarized in the attached figure.
In addition to the known effect of salt on Th17 cells, dietary salt impacts the immune system in many other pathways. The entire family of white blood cells, the soldiers of defense against external aggression by microorganisms, is impacted by dietary salt. In the recent research, the dendritic cells and regulatory cells (Tregs) carry messages to the granulocytes and macrophages. The defense function of both these cells has been demonstrated to be decreased which means increased vulnerability to infections.
In the currently reported research from University of Bonn, human volunteers and experimental animals demonstrated higher susceptibility to infections. On a high salt diet consisting of merely two hamburgers, the white blood cells in these volunteers demonstrated less antibacterial function. In mice, pyelonephritis by E. coli was persistent and aggravated in one experiment. In another experiment, Listeria infection was systemically induced and bacterial counts in the liver and spleen were measured to be dramatically higher in mice fed with salt.
In summary, research across the Globe from several prestigious institutions raises concerns regarding the impact of dietary salt on the human immune response causing decrease in resistance to a variety of infections including COVID-19. Once infected, the exaggerated autoimmune response once again influenced by dietary salt leads to higher mortality. There is however good news. If we engage in salt reduction in our diet aggressively and sincerely, there is hope for reduction of many salt related health problems affecting everyone.

Recommended Further Reading:
• Wu C et al. Induction of pathogenic TH17 cells by inducible salt sensing kinase SGSK1. Nature 2013; 496: 513-517. https://www.ncbi.nlm.nih.gov/pubmed/23467085
• O’Garra and Vieira. Regulatory T cells and mechanisms of immune system control. Nat Med 2004; 10(8):801-805. https://www.ncbi.nlm.nih.gov/pubmed/15286781
• D’Andrea MR. Add Alzheimer’s to the list of autoimmune disease. Med Hypotheses 2005; 64: 458-463. https://www.sciencedirect.com/science/article/abs/pii/S0306987704004864
• Salt is the new culprit in auto immunity; Medicine @Yale 2013-May-June,
https://medicine.yale.edu/news/medicineatyale/salt-is-new-culprit-in-autoimmunity/
• Afsar et al. Salt Intake and Immunity (Brief Review), Hypertension 72:19-23, 2018 https://www.ahajournals.org/doi/pdf/10.1161/HYPERTENSIONAHA.118.11128
• Jobin, K et al. A high-salt diet compromises antibacterial neutrophil responses through hormonal perturbation. Sci Transl Med.
https://pubmed.ncbi.nlm.nih.gov/32213629/
• Rakova et al. Increased salt consumption induces body water conservation and decreases fluid intake; J Clin Invest. 2017;127(5):1932–1943 https://www.jci.org/articles/view/88530
• Kitada et al. High salt intake reprioritizes osmolyte and energy metabolism for body fluid conservation. J Clin Invest. 2017;127(5):1944–1959 https://www.jci.org/articles/view/88532
• Bailey, Matthew et al. The relationship between salt and glucocorticoids: implications for salt-sensitive hypertension: University of Edinburgh publication, May 1, 2019. https://www.ed.ac.uk/cardiovascular-science/research/research-themes/hart/hart-research-projects/salt-glucocorticoid-relationship
• Kirabo et al. High Salt Activates Human Monocytes and Promotes their Conversion into Dendritic Cells via Formation of Immunogenic Isoketal-adducts. FASEB Journal. 30:(1) Supplement, April 2016. https://www.fasebj.org/doi/abs/10.1096/fasebj.30.1_supplement.1216.4
• Neravetla SR, Neravetal SR (2015). Table Salt and Dementia. In: Diet and Exercise Cognitive Function and Neurological Diseases. Wiley Online Library (eds: T. Farooqui and A.A. Farooqui). https://doi.org/10.1002/9781118840634.ch8

Dr. Reddy,
YOu are a crusader. But early on all prophets called out in the wild. When enough people heard them they became Saints.
Parmesh Erramilli